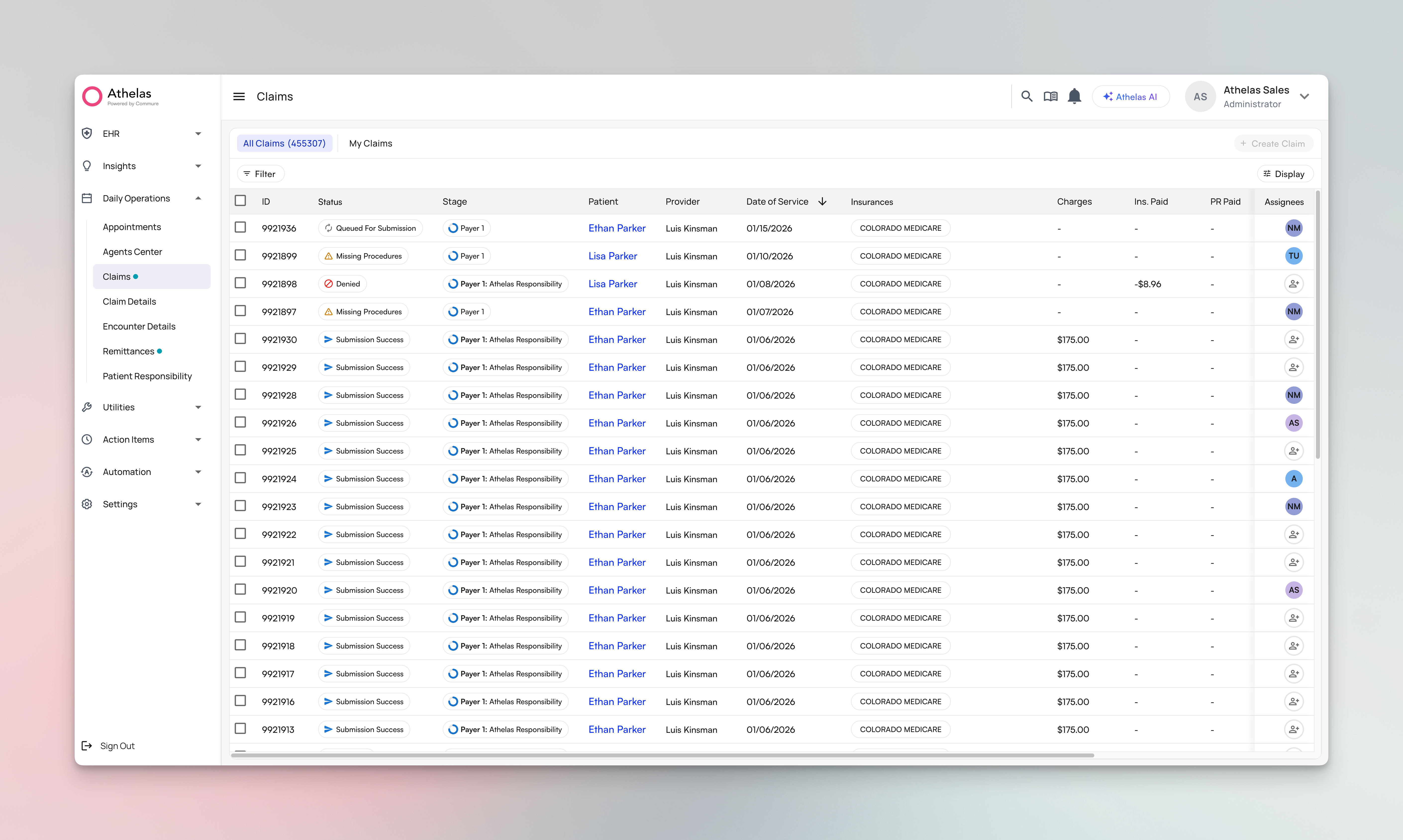
Why We Built This
Managing claims is complex. Depending on your practice size, your team juggles hundreds or even thousands of encounters on a weekly basis, each requiring detailed review, coding, and submission on repeat. (Note: In Athelas, an encounter represents a patient visit, while a claim is the billable submission created from that encounter.) We’ve heard your feedback, and the new Claims Page addresses and improves many aspects of the claim editing/submission workflow.What’s New
1. Powerful Filtering and Custom Views
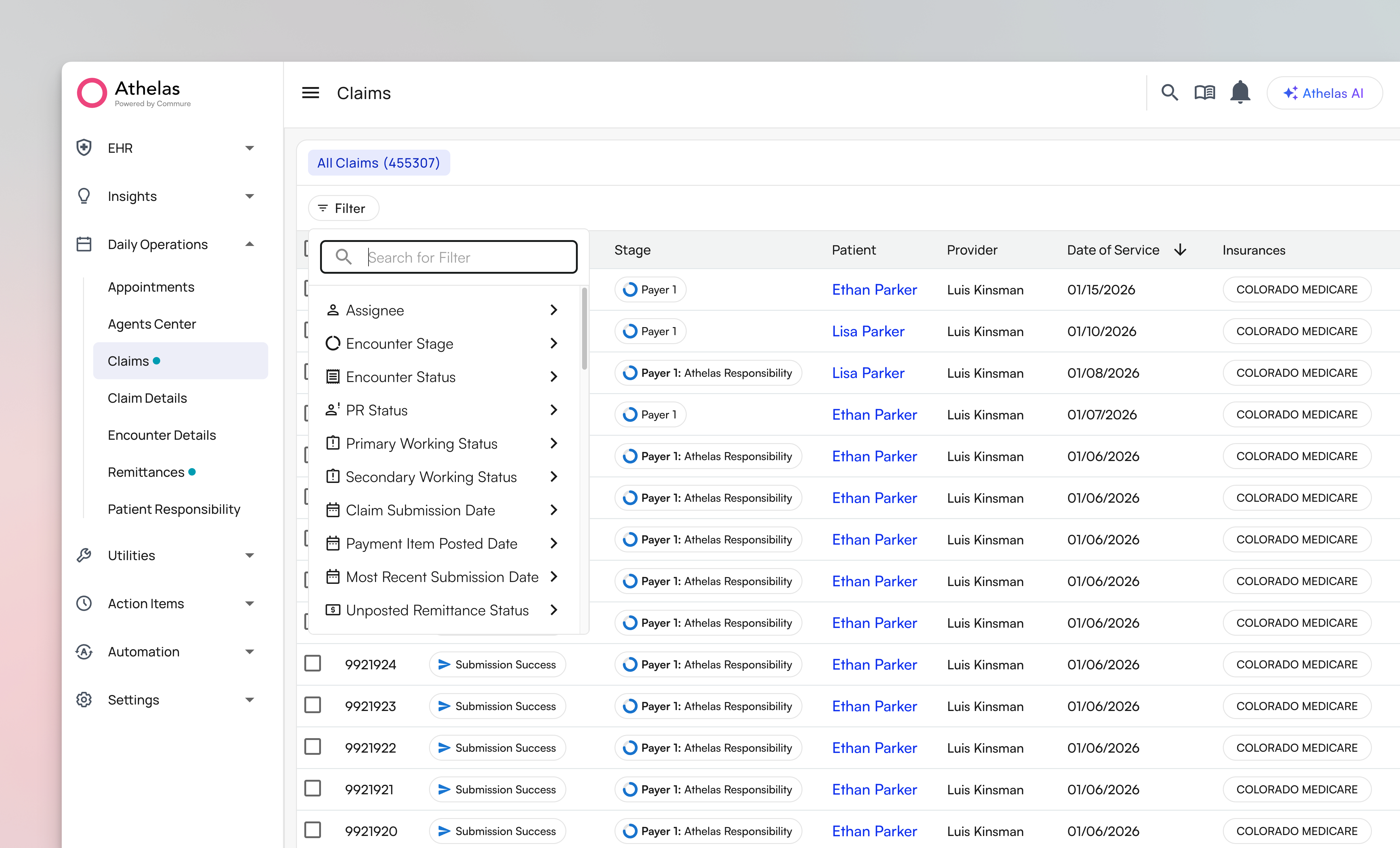
- Filter by encounter status, insurance provider, claim amount, age, and dozens of other attributes
- Sort by date of service, charge amount, provider, or any field that matters to your workflow
- Save custom views for yourself and your team (all views are user-specific; managers can filter by claims assigned to a user, but cannot see billers’ individual views)
2. Assignment Management That Works with You
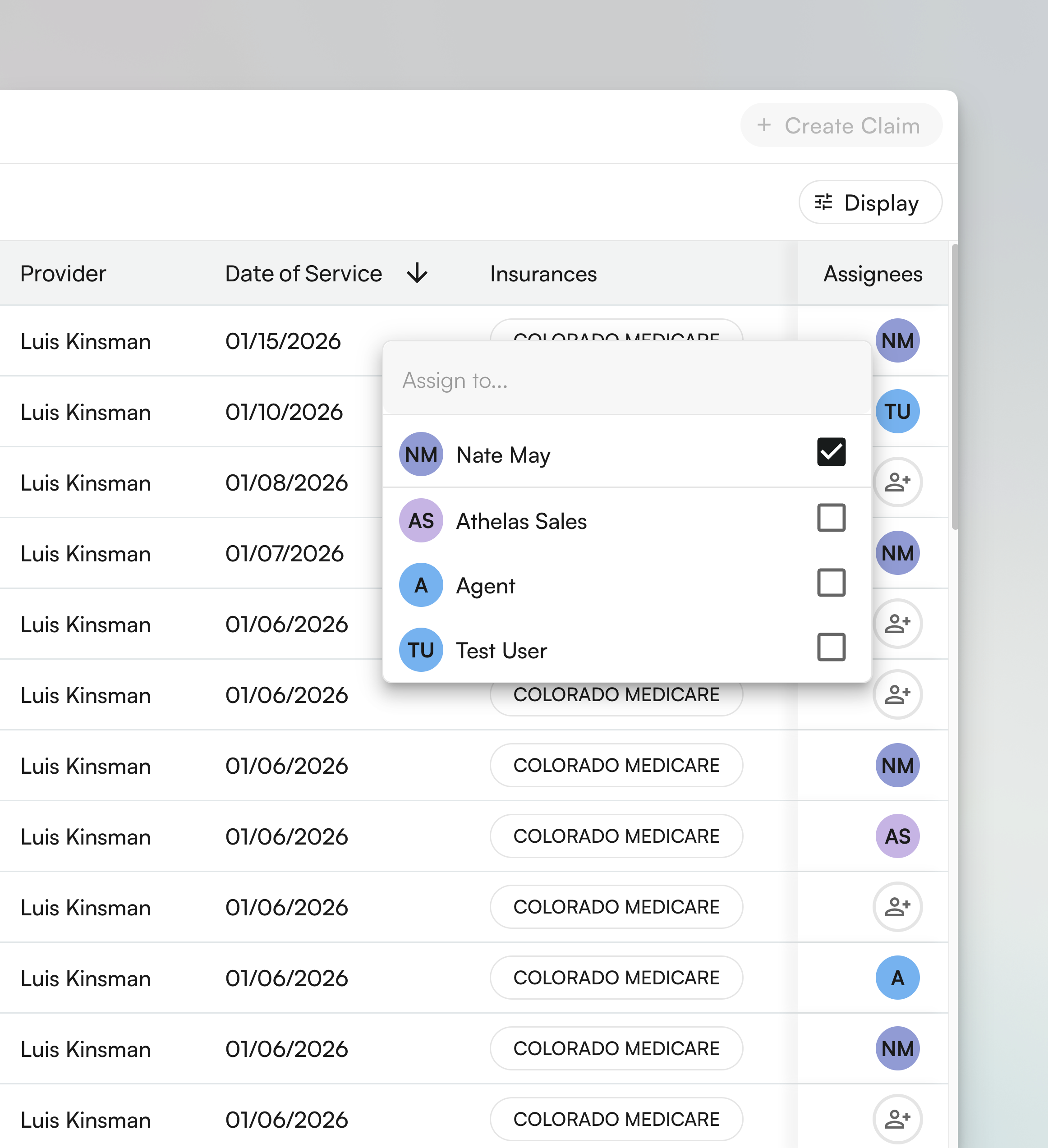
- Assign claims to specific team members with one click
- Bulk assign multiple claims to balance workload across your team
- Track who’s working on what to prevent duplicate effort
3. Smarter Claim Review with AI Assistance
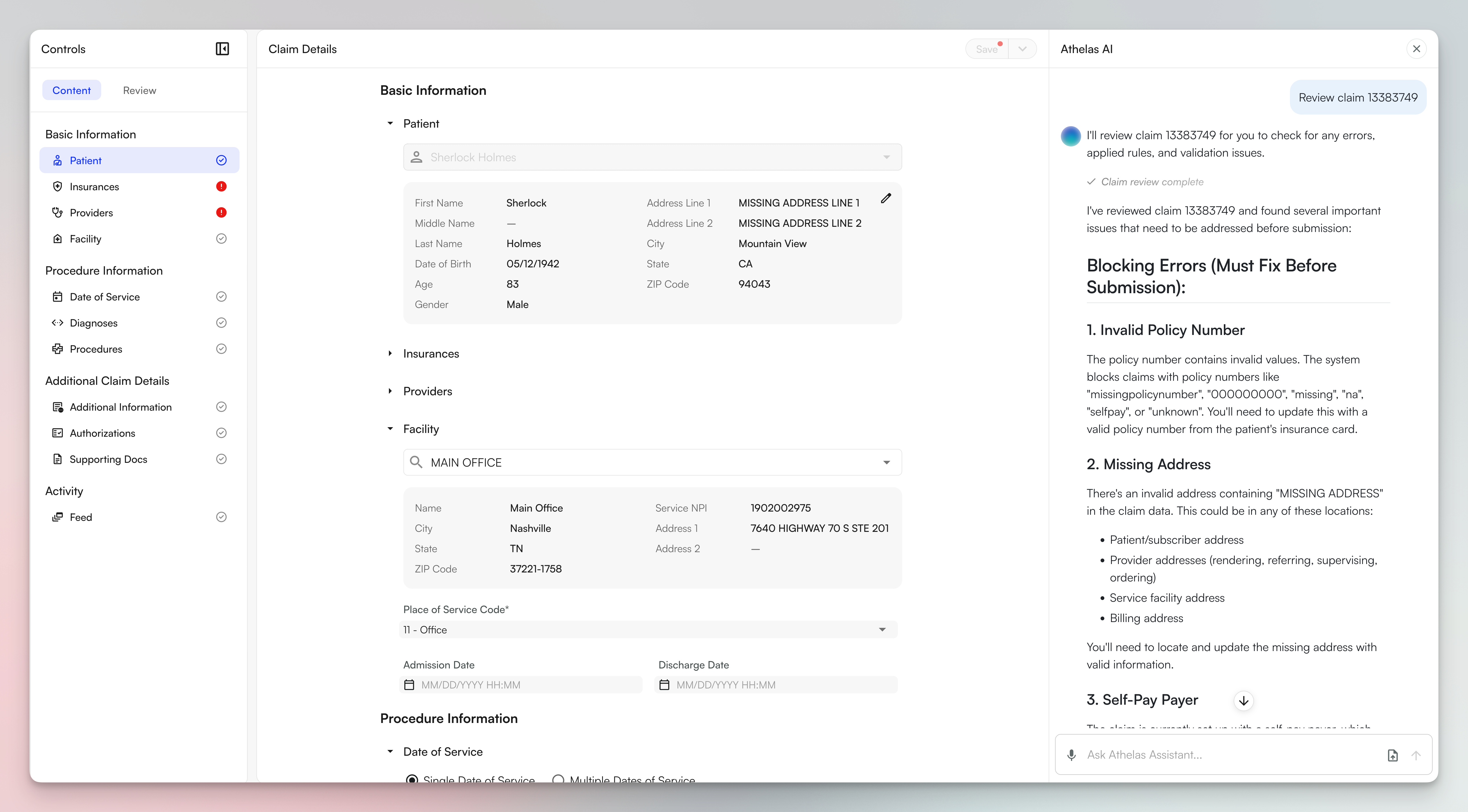
- Catch errors instantly: Missing information is flagged immediately on the content tab, no more hunting for incomplete fields
- Preview changes before submission: The new sparkles icon now shows exactly where billing rules modified the claim: correcting zip codes, adding modifiers for accurate reimbursement, and more. Review the logic behind each change and understand why before you submit.
- Block bad data automatically: We run every claim through a series of checks with our clearinghouse partners & global rules. Athelas is constantly building on based on common rejection/denial reasons, and customer-specific rules configured just for you to ensure that all claims go out clean, and as you intended.
4. Review, Collaborate, and Submit with Confidence
-
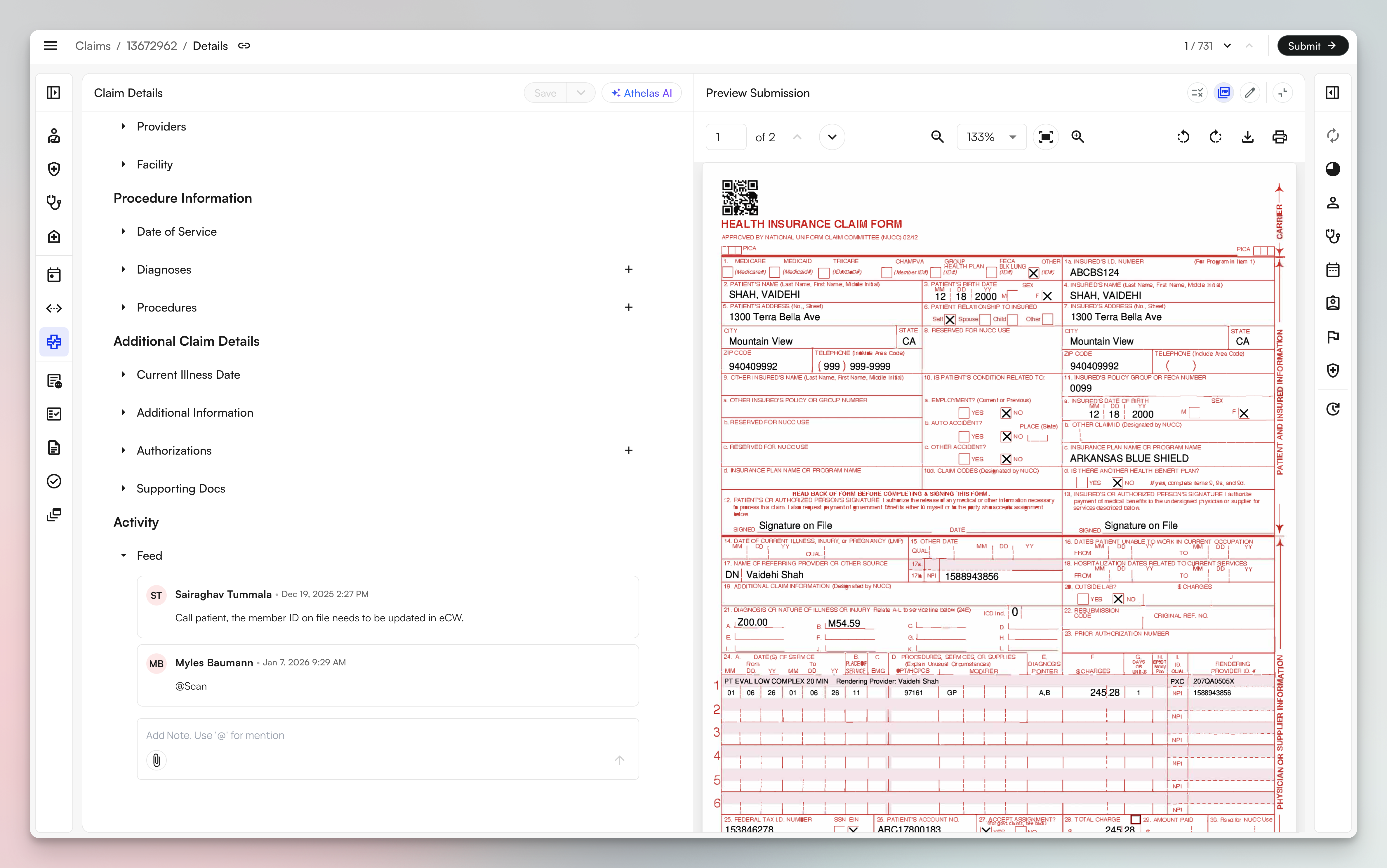
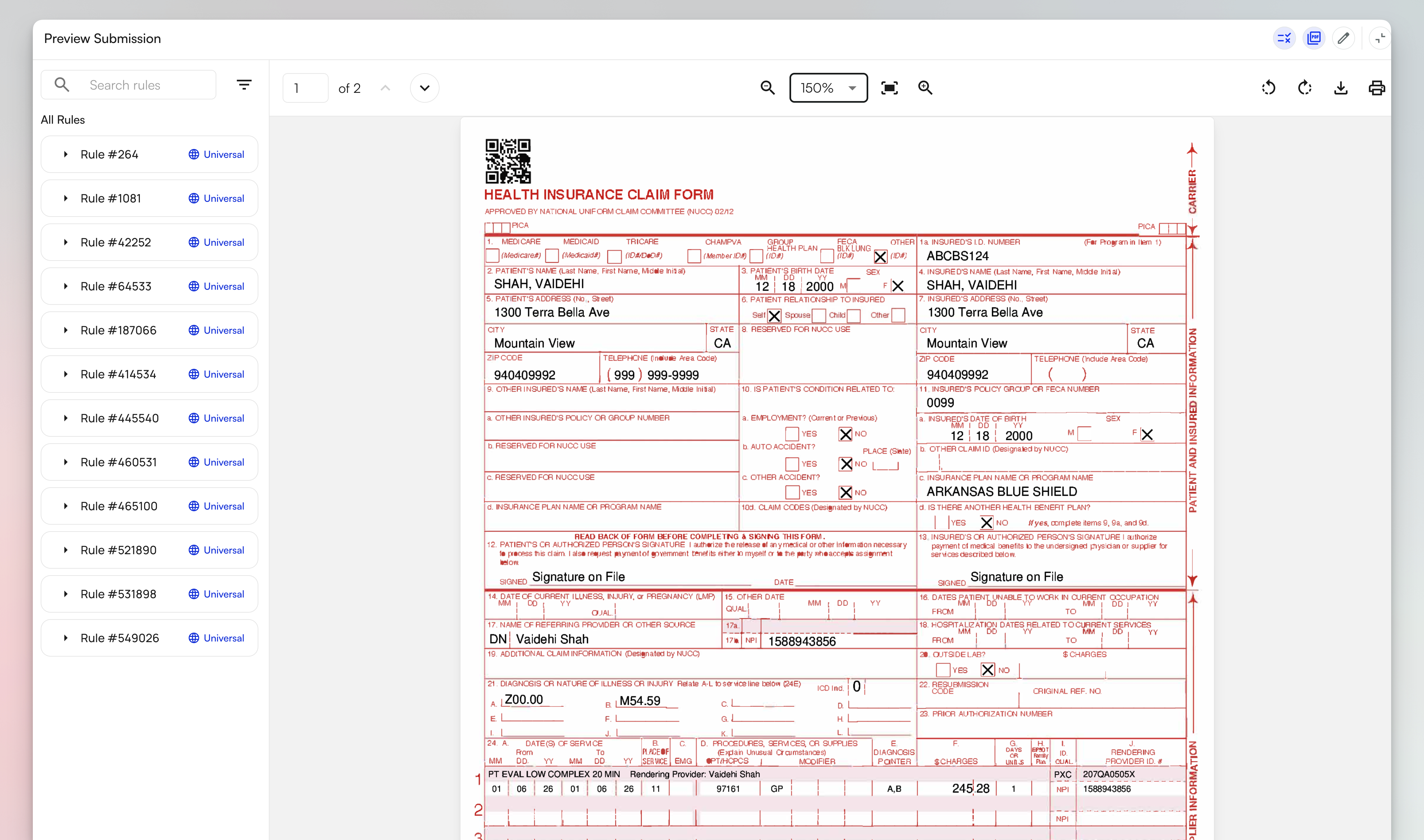
Preview changes in standard view or as PDFs (CMS-1500, UB-04, and ADA forms) before submission
-
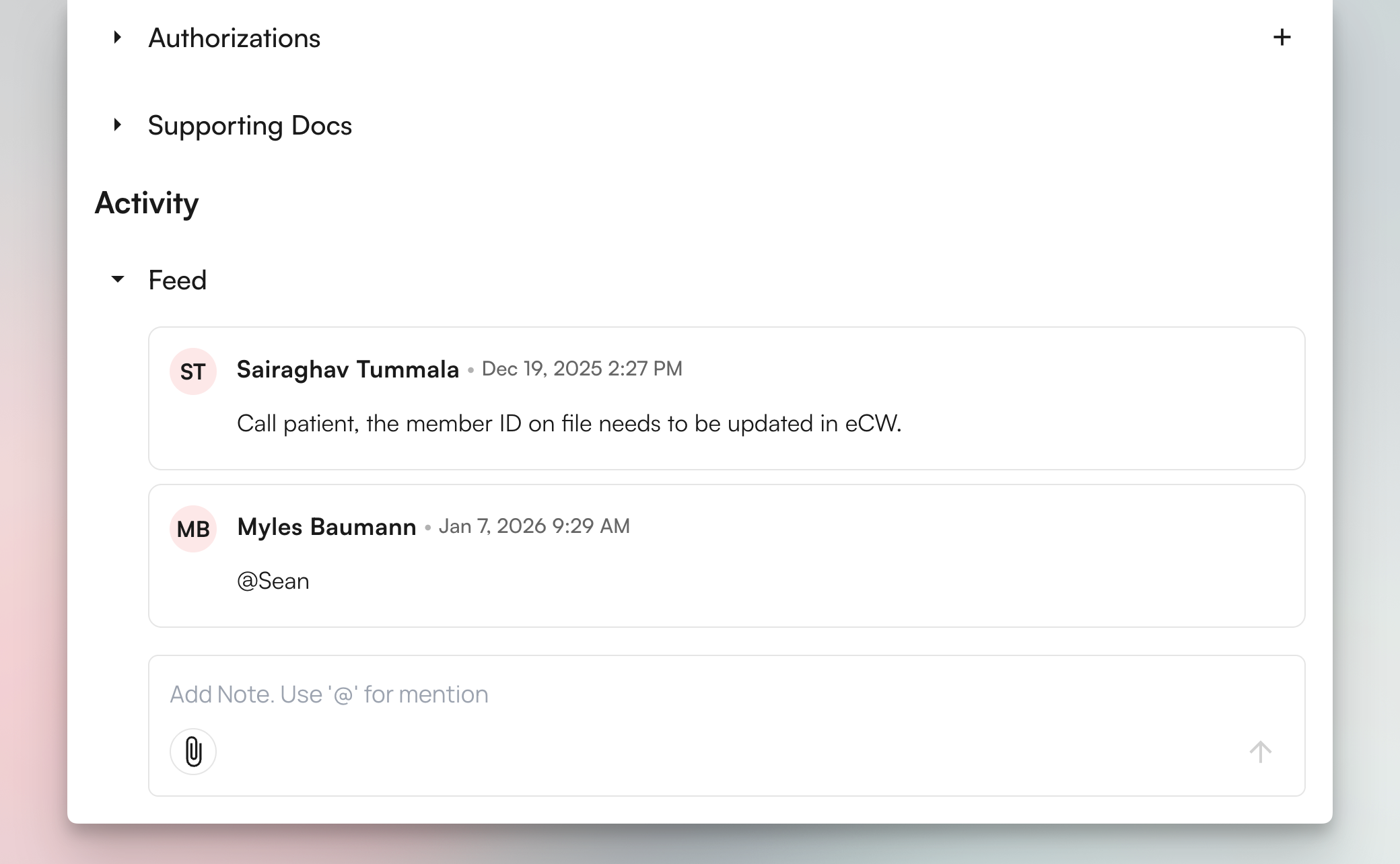
See team member’s comments directly through the activity feed
What This Means for Your Team
Fewer errors. Our AI-powered validation, rule engine, and verification steps catch issues before submission, which reduces rejection rates and rework. Faster throughput. With better navigation, bulk actions, and automated improvements, your team can easily process more claims per day. Better load balancing. Assignment tracking and bulk assignment help distribute work evenly and ensure nothing falls through the cracks. Spend less time waiting and more time working. All these features were designed to help you self-diagnose problems more quickly, so that you can get claims out faster.What’s Coming Next
This is just the beginning. Here’s what you can expect from us next:- Enhanced activity feed: Richer collaboration features and more detailed claim history
- Smart grouping: Group claims by denial reason, insurance company, or other attributes to work in batches
- Better status clarity: Improved pre-submission encounter statuses and filters so you can instantly see what’s ready to submit vs. what’s still in progress.
